iKeloid ™, A Novel Approach in Treatment of Keloids in San Antonio and Boerne Clinics of Texas Institute of Dermatology
To Schedule click here , call 210-698-6777 or email [email protected]
- Treatment of Keloids in San Antonio and Boerne Offered at Texas Institute of Dermatology Clinics
- Our renowned dermatologists offer a comprehensive approach for treatment of Keloids and Scars
- At the Keloid Clinic, our experts have successfully treated hundreds of patients with keloids by iKeloid™
- iKeloid™ consists of a specific corticosteroid injection, Cryo Keloid destruction plus laser or light treatment to address itchy painful unsightly growths
- iKeloid™ is one of the most comprehensive treatment approach for keloid scars offered at Texas Institute of Dermatology
- iKeloid™ usually inhibits new collagen formation; and let the keloids to shrink gradually combined with resurfacing the overlying skin
- Dr. Ghohestani, a renowned dermatologist with years of experience in treating keloids carefully examine each keloid patient and design a plan specific for each patient based on the site, size, among other factors
- Each Patient May Need Several Treatment Sessions to See a Significant Reduction in Size of his/her Keloids
- Once the Keloid is Shrinked in Size, a Discoloration May Persist for a Longer Period of Time; and it Requires a Conservative Treatment with Light or Laser
Before development of iKeloid™, most dermatologists or plastic surgeons offered injection or surgery which may not necessarily enough to address severe forms of keloid Scars or cause the keloids to re-appear at a larger size. With iKeloid™ your keloid scars significantly improve after receiving these cutting-edge techniques that are specifically designed for Keloid Scars. Our experts emphasize for treating Keloids, one must be very patient and
The skin is the largest organ in the body and the most susceptible to injury. When these injuries occur, depending on their depth and severity, a scar will appear. A Keloid is an excess growth of scar tissue most often located at the site of a wound. These scars are a benign form of neoplasia, meaning that they are a result of over-active cells producing more than what is necessary. This neoplasia trait often makes Keloid scarring difficult to treat.
What causes Keloids?
Keloid scars are thought to be genetically passed on. More research needs to be done in order to deduce the exact reasons why some are genetically predisposed to develop Keloid while others aren’t. Studies have shown that the disease is more common among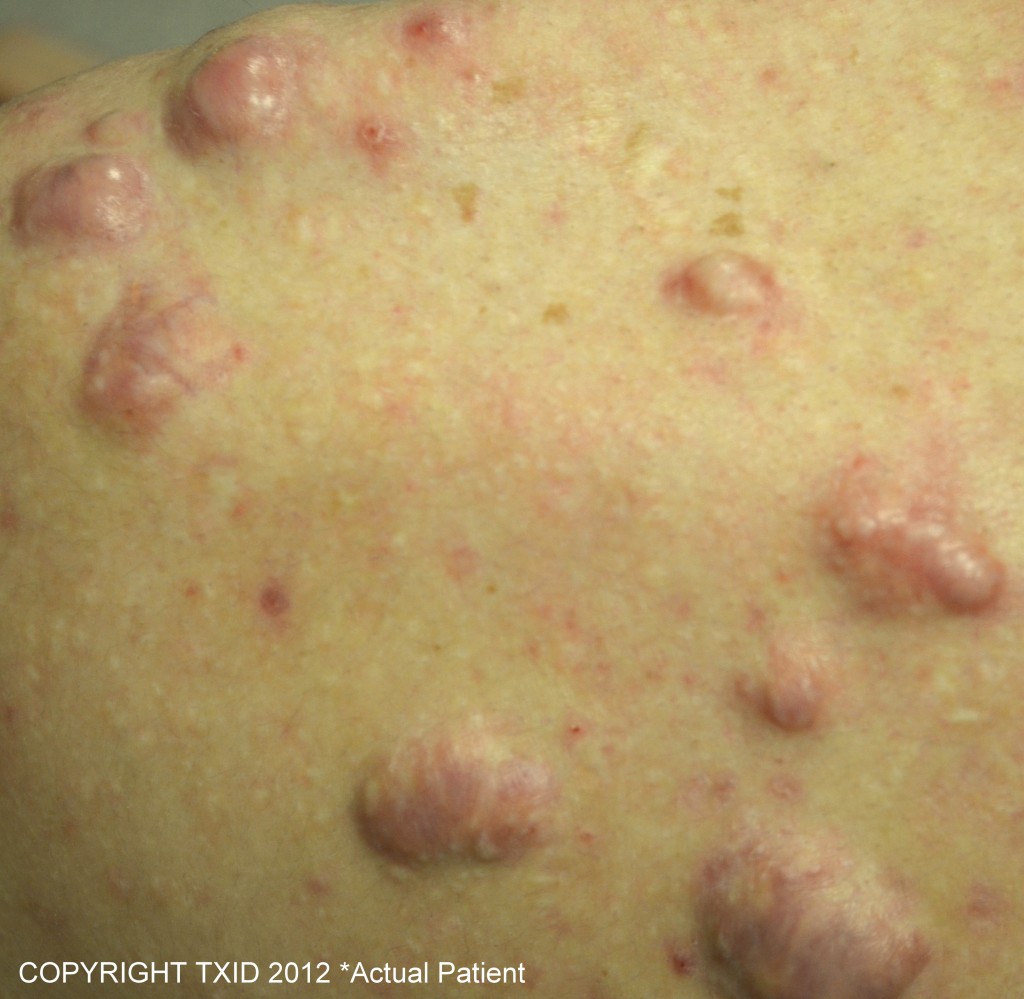 Africans, African Americans, and Asians. We do not currently know why this is the case, although many scientists believe that there may be a tie between skin pigmentation and Keloids as Albinos are free from developing this skin abnormality. Studies have also shown that Keloids tend to show more rapidly around puberty in young individuals, although Keloids can develop at any age.
Africans, African Americans, and Asians. We do not currently know why this is the case, although many scientists believe that there may be a tie between skin pigmentation and Keloids as Albinos are free from developing this skin abnormality. Studies have also shown that Keloids tend to show more rapidly around puberty in young individuals, although Keloids can develop at any age.
What are my treatment options?
Keloid treatments vary depending on the severity and type of keloid scarring, site of keloids. Following treatment options are currently available for treating keloids:
- Kenalog injection to inhibit fibroblastic activities and smoothen the surface of scar
- Cryodestruction (the application of extreme cold) method with either cryospray or cryocontact™ to shrink and debulk the keloid. In fact, Dr. Ghohestani’s team as well as Dr. Tirgan’s from New York were among pioneers of re-introducing this technique as a gold standard for treatment of most of Keloids
- AFT laser light treatment to reduce redness and shrink blood vessels around the Keloids
- LED light to decrease inflammation
- Surgery – While Keloids can simply be surgically removed, surgery in most cases is not successful. Keloid scars are a response to injury to the skin; a surgical excision is considered an injury too. Therefore, depending on the surgical technique and the site, the Keloids may come back even at a size much larger than before
- Steroid Injections – Kenalog injection in conjunction with cryofreeze may shrink keloids. Sometimes, the injection can be done for preventing keloid formation. These shots are introduced at the site of the keloids early in its development phase in order to counter-act the over-active cells that lead to Keloid formation
- Chemotherapy drugs – Keloid acts similarly to cancer. Therefore, cancer treatments like methotrexate have proven to be effective in some Keloids. The chemotherapy can be done on a case-by-case basis and may not be the best course of action for many patients
Less Desirable or ineffective Treatment Options:
- Radiation therapy such as SRT-100™ is effective yet increases chance of cancer. When safe treatment options such as cryofreeze is readily available, using radiation therapy SRT-100™ should be reserved for isolated cases, only a few. Close follow-up to detect early signs of skin cancer and other cancers highly recommended in case of radiation therapy. Furthermore there is a high recurrence rate post-radiation of keloid.
- Mederma™ cream proves to be ineffective in treating keloids or Scars. Mederma™ cream claims to contain onion extracts, there are no reliable double blind studies showing efficacy of Mederma in treating keloids
- Tea Tree Oil has no effect whatsoever on keloids, therefore it is recommended to not use Tea Tree oil for Keloids. Some cases may develop significant irritation following application of tea tree oil.
- Silicone gels are not very effective and could be costly
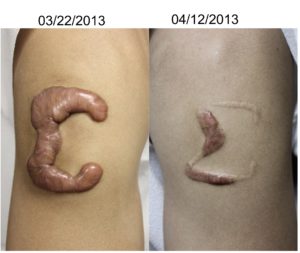
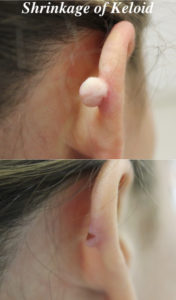
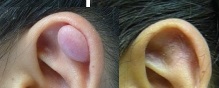
Recent Research Studies on Keloids, What’s New?
Researchers continue to study keloid scarring to better understand its origins and causes. Currently, the causes of formation and why some individuals are more prone to keloid scars than others remains unknown. Researchers have found, however, that keloid scarring tends to run in families, African Americans and Asians tend to be at a higher risk of developing keloid scars. Fore more details, please click here.
For Clinicians:
Texas Institute of Dermatology in collaboration with Keloid Research Foundation organizes an international meeting on keloids and scars in Beijing in 2019. Research scientists, dermatologists, ENT specialists, and surgeons get together from around the world from Sydney, Australia to Agadir, Morocco (more than 48 countries) to discuss latest development in pathophysiology and treatment of Keloids and Scars. For more information, please click here.
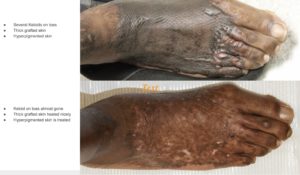
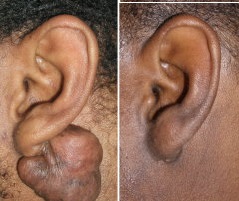
*When you review the before and after images, please note that each patient’s experience may be different. We can not guarantee that despite all our efforts, each patient may see their keloid to completely disappear, some may require several sessions; some may notice some discolorations. For more details, please review our treatment consents or call us at 210-698-6777.
******
Why choose the Texas Institute of Dermatology for your Keloid treatments?
Our mission is to serve as a leading center for understanding and treating skin, hair, and nail diseases in South Texas through excellence in patient care, research, and education. We want you to feel that you have been treated with the comfort, privacy, safety, and satisfaction that you deserve. This is why all of our procedures are performed or supervised by our renowned dermatologist, Dr. Reza Ghohestani. His experience, combined with the latest technology and caring staff, is why the Institute is consistently ranked among the top dermatology centers in San Antonio and Boerne areas based on satisfaction surveys. We currently serve communities throughout Bexar and Kendall counties, including San Antonio, Boerne, Leon Springs, Fair Oaks Rank, Canyon Lake City, etc. Many of our patients also come from San Marcos, New Braunfels, Kerrville, Austin, Wimberly, and Corpus Christi.