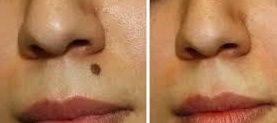
Mole Removal in San Antonio by Top Ranked Dermatologists
To Schedule Click here , Call 210-698-6777 or Email [email protected]
- We Offer latest technology for Safe Mole Removal in San Antonio and Boerne Clinics
- Our Mole Experts Carefully Examine Moles with Moloscope™ to Distinguish the Benign from the Malignant Moles
- Some Moles May Require a Biopsy to Ensure that They are not Malignant
- Dermatologists with Expertise in Moles May Accurately Determine Which Moles Are the Dangerous Ones (Malignant)
- Our Mole Experts have successfully removed thousands of moles with minimum or no scars
- At TXID San Antonio Mole Clinic, you will be seen by our renowned dermatologists who have years of experience in diagnosing and treating various types of moles (benign or malignant)
- State-of-the art technology combined with our Dermatologists’ expertise offer a desirable outcome with minimal scars for removing the moles
- We offer local anesthesia so the mole removal could be as painless as possible
- Our Mole experts with years of experience in detecting various type of Moles will discuss with you the best treatment options designed for your mole based on the nature of mole (epidermal, compound or dermal, benign or malignant) and location of the mole (face, back or chest etc). Approach to a deep mole on the face is different from a flat mole on the back.
- Our Mole experts are ranked among the top Dermatologists in San Antonio and Boerne with expertise in removing moles with minimal scars
- After the mole removal, the specimen is evaluated by a dermatologists and then sent to a pathologist to examine it under a microscope.
Moles, What Are They:
“Nevi” (singular = nevus) is the more scientific term used to describe moles, which are common among humans and tend to increase in number until we reach the age of 30. Moles are result of melanocytic cell proliferation in skin. The majority of these moles are benign, meaning they are not cancerous. Generally speaking, these moles do not pose a significant threat to health. Over time they will transition from flat spots, to raised lesions, and often to a soft, fleshy growth. However, in some cases, these moles may change in size, color, or may simply be very large. The warning signs for malignant melanoma (a fatal skin cancer) are listed below. Dr. Ghohestani recommends that individuals with a large number of moles or moles that meet the criteria described below should schedule an appointment for a skin exam with a dermatologist. To schedule an appointment, call us at (210) 698-6777.
Moles: Benign or Malignant?
All Moles are not the same. It is important to distinguish a benign Mole from a Malignant Mole. People may not be aware of importance of removing the entire margin around malignant Moles. If a small piece of Mole left behind, it may regrow and extend to other areas. Partially treated and untreated Malignant Melanoma lesions may spread to other areas. Therefore, it is of utmost important that each mole is submitted for pathology for microsopic evaluation after its removal according to Dr. Ghohestani, Director of Texas Institute of Dermatology.
Congenital Mole:
Congenital moles referring to moles that are present at birth. These moles can vary significantly in size from very small to very large. Research has shown that large congenital moles (greater than 10 cm) are at a higher risk of developing into Melanoma (a deadly skin cancer). If you have a large congenital mole, make sure to schedule an appointment with a dermatologist for a skin exam.
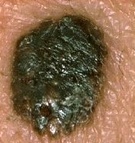
Atypical or Dysplastic Mole
Moles that are larger than a pencil eraser and/or are irregular in shape may require further inspection under a microscope in order to detect early signs of cancer (known as dyplastic nevus). These types of moles generally are darker in the center and lighter around the edges. Early detection is critically important in order to avoid the onset of melanoma, a deadly form of skin cancer. Any changes in mole color, shape, and/or size should be checked by a dermatologist in order to detect skin cancer.
Benign Mole
Acquired benign moles are ones that are not present at birth, hence the name. Individuals with more than 50 acquired moles may be at a higher risk for melanoma than those with fewer moles.
Anyone who has a mole with atypical features (see below) should see a dermatologist regularly, perform self-exam, and practice sun protection.
What are the Danger Signs?
Danger Signs of Mole . According to Dr. Ghohestani, a dermatologist with years of experience in treating cancerous lesions and Malignant Moles: “everyone should be aware of danger signs for Melanoma”. No moles should be subject to freezing or laser without determining whether it’s a benign or a malignant?
Research has shown that moles with certain features have higher-than-average risk of becoming cancerous. Click here to see and print a user friendly sheet to help map your moles for your future dermatology visit and Mole check.
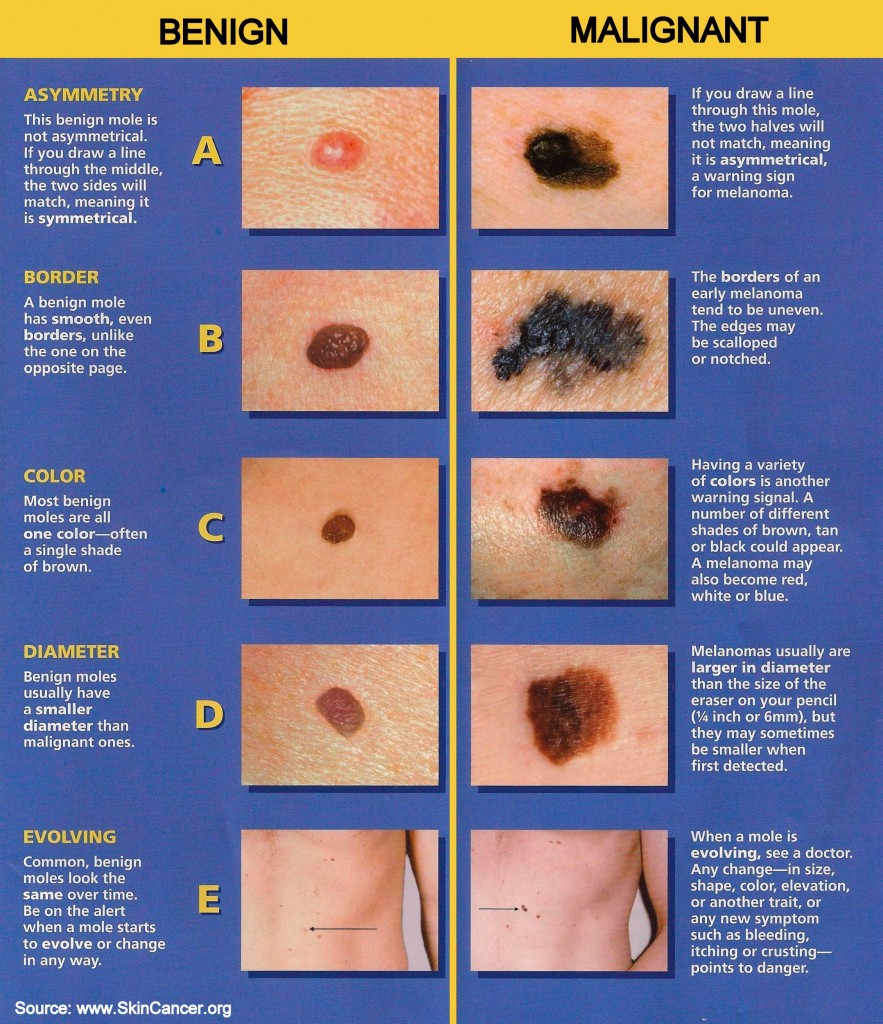
Performing regular skin self-exams helps people recognize the early warning signs of melanoma. Dermatologists recommend that everyone perform regular skin self-exams. When examining your moles, look for the danger signs:
- A stands for ASYMMETRY; one half unlike the other half.
- B stands for BORDER; irregular, scalloped, or poorly defined border.
- C stands for COLOR; varied from one area to another; shades of tan, brown, and black; sometimes white, red, or blue.
- D stands for DIAMETER; melanomas are usually greater than 6mm (the size of a pencil eraser) when diagnosed, but they can be smaller.
- E stands for EVOLVING; a mole or skin lesion that looks different from the rest or is changing in size, shape, or color.
As you examine your skin, it is important to know that not all moles look alike. Even in the same individual, moles can differ in size, shape, or color. Moles can be flat or raised. The most common colors range from tan to brown, but moles can be pink, black, blue, or even skin-toned. Moles can have hair. Some moles will change slowly over time, possibly even disappearing.
Be sure to examine your entire body. Moles can appear anywhere on the skin. Moles develop on the scalp, between the fingers and toes, on the soles and palms, and even under the nails.
A dermatologist should examine any mole that stands out from the rest. This includes any spot that changes in size, shape, or color, and any lesion that bleeds, itches, or becomes painful.
Which Moles Need to be Checked?
The majority of moles do not pose any immediate threat. The moles of greatest concerns are ones that fall under the detection signs spoken of above. These moles are ones that are large in size, darker than the others, look different than other existing moles. Any changes in height, shape, color, or size should be checked out by a dermatologist. If the mole begins to bleed, itch, ooze, appear scaly, or become sensitive to touch or painful, immediately call your dermatologist to schedule an appointment.
Regular examination facilitates early detection. Areas exposed to the sun (i.e. face, ears, neck, chest, hands, arms) are at the highest risk for developing melanoma.
To schedule an appointment, call us at (210) 698-6777 or email us at [email protected].
What are the Treatment Options for Moles and Benign Skin Growths?
- Surgical removal, usually the excision (cutting the skin using a blade) will be carefully done along the Blaschko lines to minimize risk of scarring
- Laser, for some benign growths such Seborrheic Keratosis
- Dr. Ghohestani and most experts do not recommend to remove a mole by laser or cauterization
- Each mole should be carefully examined under a microscope after removing it
Early signs of malignant moles can only be determined under close examination through a microscope by a dermatologist. Many studies showed that more than 50% of non-dermatologists physicians may not accurately distinguish a malignant mole from a benign mole. For this reason, any moles in question will be examined by Dr. Ghohestani, a top ranked San Antonio Dermatologist, or a member of his staff to ensure that early warning signs are not present.
If the mole is cancerous, Dr. Ghohestani will remove the mole and have it checked under a microscope. According to Dr. Ghohestani who has more than 25 years of clinical experience, all moles should be sent for a thorough microscopic exam. Sometimes, a mole may not be dark and mimic a benign, normal looking. Later the microscopic exam shows it is cancerous such as amelanotic melanoma.
The most common removal method for moles is surgical excision, which means Dr. Ghohestani will cut the entire mole from the skin and stitch the skin closed. Shaving is another removal option where, using a surgical blade, the dermatologist shaves the mole away from the skin. Neither of these methods should be attempted at home. Removal of a mole in a dermatologist’s office is a simple, safe procedure that can be accomplished in a standard office visit. All samples must be examined under microscope. If the mole is found to be cancerous, Dr. Ghohestani or a member of his staff will contact you to discuss treatment options. If the mole grows back after the excision or shaving, another appointment should be made immediately.
How Can I Prevent Getting Moles?
Moles are usually formed spontaneously, based on your genetic background. Currently, there is no any available preventive measures to avoid getting benign moles. Vigilance and protection are the two greatest tools we have against malignant moles. Routine skin inspections facilitate early detection. Any changes to existing moles and any additional moles should be reported to your dermatologist. Dr. Ghohestani recommends regular skin examinations by a dermatologist, especially for those with high risk factors for cancer (i.e. family history of skin cancer, individuals with excessive sun exposure). Apart of the family history, the most prevalent risk factor for skin cancers is sun exposure specially for South Texas residents including San Antonio, Boerne and Laredo. Practicing safe sun and regular skin check are the best preventative care for skin cancer. Practicing safe sun includes:
- Apply a broad-spectrum water-resistant sunblock with a Sun Protection Factor (SPF) of 30 or more to all sun-exposed skin. Certain sunblocks are better than others. Click here to learn more. Reapplication is the most commonly missed element of applying sunblock. Dr. Ghohestani recommends re-application every two hours or immediately after swimming or sweating.
- Wear protective clothing. Protective clothing includes pants, wide-brimmed hats, long-sleeved shirts, and sunglasses.
- Seek shade. The sun’s rays tend to be the most intense between 10 AM and 4 PM. As a general rule of thumb, if your shadow is shorter than you are, seek shade.
- Protect children from the sun. The three tools listed above apply to children as well as to adults.
- Use extra caution when playing in the water, snow, and/or sand. Many do not realize that water, snow, and sand can reflect the damaging rays of the sun, which can increase your chances of sunburn.
- Avoid tanning beds. Excessive exposure to the Ultraviolet rays from the sun and from tanning beds leads to skin cancer and wrinkling. Sunless self-tanning products are a safe alternative to UV tanning and provide the desired color. Sunscreen should still be used on top of the self-tanning product.
- Check your skin on your birthday. Dermatologists recommend at least a once-yearly personal skin exam in addition to a yearly skin check performed by a dermatologist. If you notice anything of concern, contact a dermatologist immediately and schedule an appointment. Treatment is easiest and most effective with early detection.
Why should you choose Texas Institute of Dermatology for mole removal ?
Our mission is to serve as a leading mole removal center in South Texas through excellence in patient care, research, and education. We want you to feel that you have been treated with the comfort, privacy, safety, and satisfaction that you deserve. This is why all of our laser procedures are performed or supervised by our renowned mole specialists. Their extensive experience, combined with the cutting-edge laser technology and caring staff translate to a superior result. The Texas Institute of Dermatology, Laser and Cosmetic Surgery is consistently ranked among the top dermatology and laser centers in the San Antonio and Boerne area based on peer reviewed satisfaction surveys. We currently serve communities throughout Bexar and Kendall counties, including San Antonio, Boerne, Leon Springs, Fair Oaks Ranch, Canyon Lake City, etc. Many of our patients also come from Laredo, San Marcos, New Braunfels, Kerrville, Austin, Wimberly, McAllen and Corpus Christi. If you are looking for a top laser for face in San Antonio or Boerne, call us at 210-698-6777 or email to [email protected].
* If the Content contained on this site contains medical or health sciences information, it is intended for answering some common skin care questions. No suggested test or procedure should be carried out without visiting a health care professional and unless, in the reader’s judgment, its risk is justified. Because of rapid advances in the medical sciences, we recommend that the independent verification of diagnoses and drug dosages should be made. NEITHER TEXAS DERMATOLOGY INSTITUTE NOR ANY OF ITS AFFILIATES OR LICENSORS SHALL BE LIABLE TO YOU OR ANYONE ELSE FOR ANY LOSS OR INJURY, CAUSED IN WHOLE OR PART BY ITS NEGLIGENCE OR CONTINGENCIES BEYOND ITS CONTROL IN PROCURING, COMPILING, INTERPRETING, REPORTING OR DELIVERING INFORMATION THROUGH THE SITE. IN NO EVENT WILL TEXAS DERMATOLOGY INSTITUTE, ITS AFFILIATES OR LICENSORS BE LIABLE TO YOU OR ANYONE ELSE FOR ANY DECISION MADE OR ACTION TAKEN BY YOU IN RELIANCE ON SUCH INFORMATION. TEXAS DERMATOLOGY INSTITUTE AND ITS AFFILIATES AND LICENSORS SHALL NOT BE LIABLE TO YOU OR ANYONE ELSE FOR ANY DAMAGES (INCLUDING, WITHOUT LIMITATION, CONSEQUENTIAL, SPECIAL, INCIDENTAL, INDIRECT, OR SIMILAR DAMAGES) EVEN IF ADVISED OF THE POSSIBILITY OF SUCH DAMAGES.You hereby agree to indemnify, defend and hold Texas Dermatology Institute, its directors, officers, shareholders, parents, subsidiaries, affiliates, agents and licensors harmless from and against any and all liability, losses, damages and costs, including, without limitation, reasonable attorneys’ fees, arising from your use of the Site or Content.